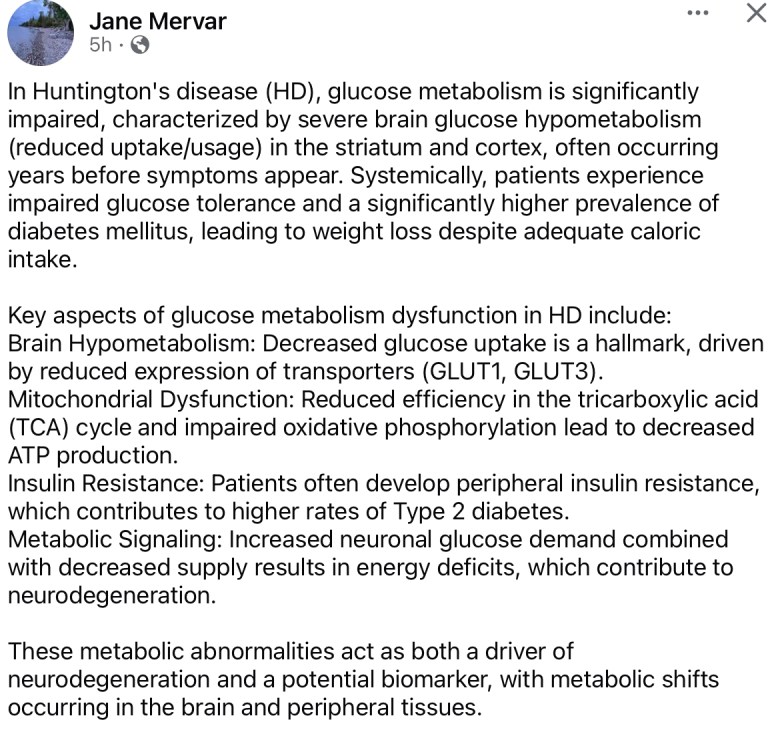
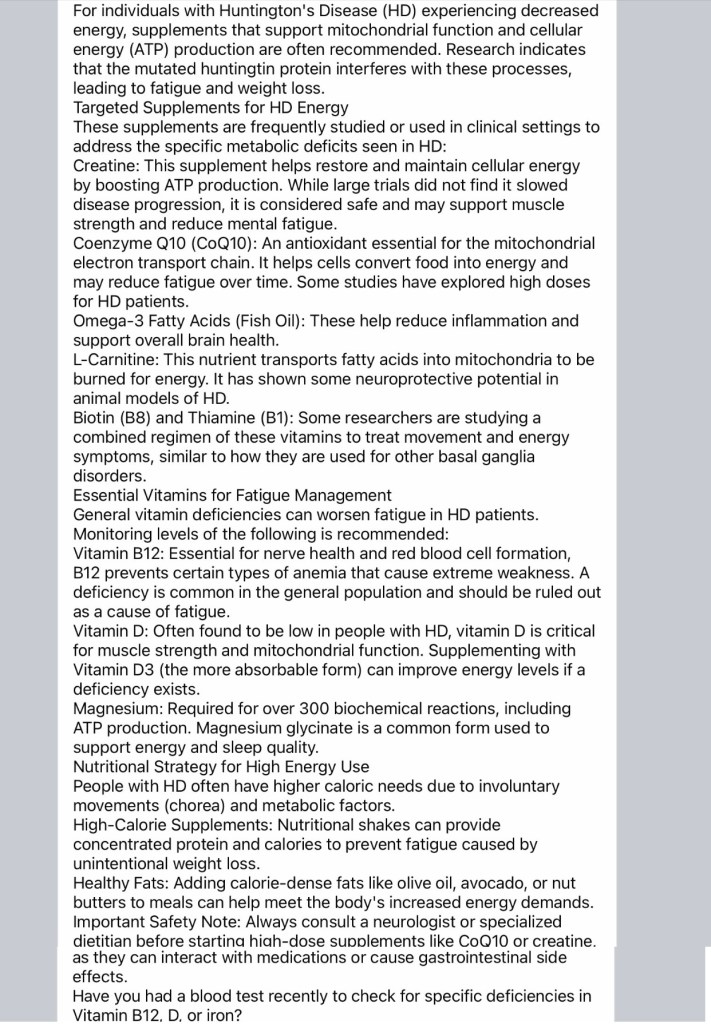
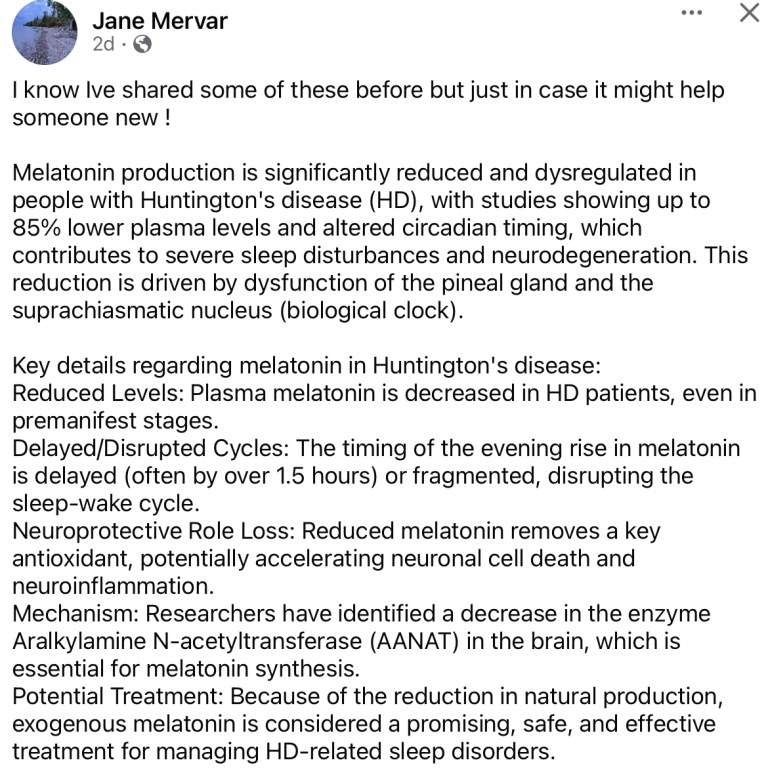
Juvenile-onset Huntington’s disease (JHD), generally defined as symptom onset before age 20, usually involves 60 or more CAG repeats. However, approximately 50% of JHD cases actually have fewer than 60 CAG repeats, with cases reported with repeats as low as 42.
Juvenile-onset Huntington’s disease (JHD), generally defined as symptom onset before age 20, usually involves 60 or more CAG repeats. However, approximately 50% of JHD cases actually have fewer than 60 CAG repeats, with cases reported with repeats as low as 42.
While a lower CAG count (e.g., 40–55) typically implies a slower progression than counts >80, a JHD diagnosis regardless of the exact repeat count (if it causes symptoms in childhood/adolescence) implies a more rapid decline than adult-onset HD, with a generally poor prognosis.
Prognosis and Progression (<60 CAG repeats)
Disease Duration: Individuals with JHD usually live about 10 to 15 years after the first symptoms appear, though some cases may progress over 10 to 30 years.
Rate of Progression: The earlier the symptoms appear, the faster the disease progresses.
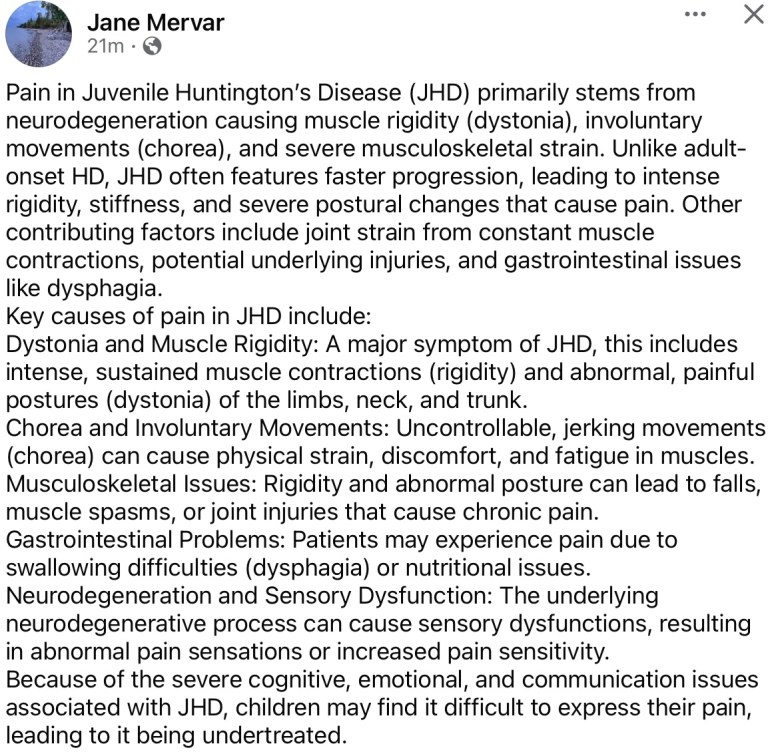
Key Symptoms: In addition to classic HD motor issues (chorea), JHD with lower repeats often presents with behavioral changes, academic struggles, and stiffness (rigidity).
Management: There is no cure, and treatment is focused on managing symptoms, such as using medication for seizures, mood swings, and rigid movements.
Key Considerations
Genetic Anticipation: JHD is usually inherited from the father, and the CAG repeat count often increases (expands) when passed from parent to child, leading to earlier and more severe disease.
Variable Prognosis: While higher repeats generally mean a more aggressive, faster-progressing disease, the exact prognosis for an individual with <60 repeats can vary, making it important to consult with specialists. Cases may progress over 10 to 30 years. It makes it hard for them to do simple things like go outside to play with their friends on the playground or even blow out their birthday candles. There are many milestones that these kids might never experience. It slowly takes away abilities and worsens and worsens until they can’t do anything, and then they sadly pass away from it.
There is NO CURE.
Please help us find one.
Symptoms may come and go and the age of development and presentation of symptoms, combined with the lack of professional experience with these kids might be factors in untimely or miss diagnosis and lack of understanding the kid’s full needs. This can cause too many difficulties for family and professionals caring for these kids.
Only an estimated ten percent of people at risk for Huntington’s Disease develop the juvenile form, but it’s hard to get accurate numbers. Juvenile Huntington’s disease (JHD), defined as HD arising before age 20, accounts for 5-10% of HD cases probably even more!! The younger the onset, the faster the progression. Which makes it harder for family, friends and even doctors to cope with.
-
A huge question might be, when should we be concerned that my kid might have JHD? Due to the variability and the truth that kids are developing and growing, and many other factors, the best answer would likely be “when there is an obvious change”, particularly one that is impacting the kid’s quality of life. There is approximately a 40% chance that someone who develops JHD will develop epilepsy. Some ways to tell if someone may have JHD are if they have a decline in school, behavior issues, personality changes ,impulsiveness, memory loss, difficulty with comprehension, balance or movement difficulties. The list could be quite long.
-
A significant question might be when should we test the kid? This has been a confusing question. The response will vary dependent upon who you speak with. NO one wants to give a kid a terminal diagnosis. A diagnosis is a quite serious step, keep in mind, diagnosed or undiagnosed if someone is symptomatic their genetics will not change. Taking the time to be sure everyone in the immediate family is as prepared as they can be is likely invaluable, while weighing the kid’s care and needs for treatment in this process also. An experienced genetics and or pediatric neurology team is important in assisting the family along with involving a social worker with the HDSA.
It’s always important to not place expectations on a kid with JHD, adapting their world to them, vs. adapting them to the world. Keeping in mind that all changes are not necessarily permanent, a kid may be unable to walk one day and then the following day walk again as if there had never been an issue. On the other hand it might become a chronic thing then is most likely the jhd. MOST IMPORTANTLY to keep in mind that just because the kid is terminally ill with a degenerative condition DOES NOT mean there is no HOPE or that nothing can help. Diagnosis is a new beginning NOT an end.
Loss of motor control will make test taking slow and confusing..
here’s amazing resources for juvenile huntington’s disease
Click This For NCIB Site
http://www.hdsa.org/images/content/2/4/v2/24235/HDSA-Juv-horiz-13e-part1.pdf
Stanford Hopes
Here’s another great one showing the widespread of jhd brain vs hd brain and progression and symptoms: Health Innovations
Kids with JHD are quite special young people with invaluable lessons to teach anyone who’s life has been touched by these kids.